The Sunday Mail

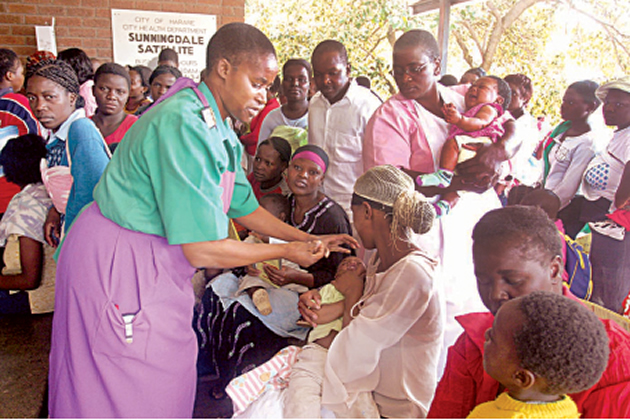
 Mrs Grace Dambanemwana, the sister-in-charge at Sunningdale Satellite Clinic, administers polio vaccine to children in the Harare suburb
Mrs Grace Dambanemwana, the sister-in-charge at Sunningdale Satellite Clinic, administers polio vaccine to children in the Harare suburbTHE number of infants dying before reaching the age of 12 months in Zimbabwe declined by 63,37 percent between 2005 and 2013, a development attributed to Government’s response to the HIV and AIDS pandemic.
The CIA World Fact Book said the infant mortality rate (IMR) decreased from an estimated 67,69 deaths per 1 000 live births in 2005 to 24,79 deaths in 2013.
IMR is an estimate number of babies below one-year-old who die per every 1 000 live births.
The IMR decline is largely attributable to introduction of prevention of mother to child HIV transmission (PMTCT) programmes.
“In 2005 IMR was at 67,69 and it decreased to 51,71 in 2006 where it had a slight decrease to 51,12 in 2007,” states the CIA Fact Book. This indicates that at least 67 infants were dying out of every 1 000 live births that took place in the country in the year 2005 before the figure declined in the following year.
“The rate further declined to 33,86 in 2008; 32,31 in 2009; 30,9 in 2010; 29,5 in 2011; 26,23 in 2012 and last year it was estimated at 24,79 deaths per every 1 000 live births.”
IMR is often also used as an indicator of the general socio-economic development of a nation.
Government and its partners have introduced a raft of effective strategies to improve healthcare delivery, mainly centralised on the national HIV and Aids response.
The Health and Child Care Ministry initiated the PMTCT programme in 1999 at three sites and then spread it countrywide.
PMTCT national co-coordinator Dr Angela Mushavi told The Sunday Mail Extra: “HIV used to be the major cause of Infant mortality as positive pregnant mothers were giving birth to infected babies and these babies would only be initiated on treatment after 18 months, which reduced their chances of survival
“Back in the day, we used antibody tests for HIV testing in both infants and adults. The testing process prolonged the whole process of early infant diagnosis (EID) as the results of the tests took long to come out.”
EID is the HIV virological testing used to diagnose infection in infants, and it is essential for ensuring for timely initiation onto anti-retroviral therapy.
In 2007, the Health Ministry introduced a new testing regime called DNAPCR, which quickened initiation of infants from 18 months to four to six days.
Dr Mushavi said, “This had an impact of increasing chances of survival for HIV-infected infants. The chance of survival for an infected infant is also determined by the existence of the mother; if the mother dies when the baby is below 12 months, the chance of survival for the baby also decreases.
“If the mother stays alive then chances of survival for the baby are bound to increase because they will be able to breastfeed their infants. Breastfeeding strengthens the infant’s immune system and prevents diseases that can kill infants such as pneumonia and diarrhoea.”
She said as years passed by, the PMTCT became more effective with the introduction of several sensitisation programs in communities that raised awareness on PMTCT.
Dr Mushavi added: “The strengthening of the PMTCT program has improved both the health of the infected mother and the health of the newborn whether infected or not.”
“Recently, we launched the Option B plus method which helped HIV infected mothers and made the program more effective. Therefore, we anticipate the IMR to continue decreasing.”
“The method keeps the infected mother alive and healthy enough to breastfeed their babies.”
On the other hand, National Aids Council (NAC) has been working hand in hand with the health ministry in ensuring that the HIV and Aids program have been strengthened to improve the overall health system of the country. NAC Monitoring and Evaluation Manager Mr Amon Mpofu has said EID results used to be prolonged as the DNA tests results would be transferred to the respective centers by road.
“Using road as a mode of transporting, DNA results of the infant was a major constrain in the EID program. This is mainly because during the long process, there were reports from health centers which suggested that the results were getting mixed up before reaching their destination,” Mr Mpofu said.
“Following the reports, NAC and the Ministry of Health initiated the message platform where the infant’s DNA tests results would be sent back to the centers using mobile messages.”
He said the initiative brought a positive change in the EID, saving many infants along the way.
However, there are other factors other than the HIV national response that have contributed to the major decline in the IMR; for instance the Health Transition Fund (HTF) programs, which are being implemented by the Ministry of Health and Child Care.
HTF is a pool of funds, sourced by the Canadian International Development, Agent Irish Aid, Norwegian embassy, Sweden, UK aid and World Health Organisation to support the national health strategy to improve access to quality health care in Zimbabwe.
Part of the fund has been supporting newborns, community health service delivery, and strengthening the Expanded Programme for Immunisation (EPI) and IMNCI and Nutrition since 2011.This has also contributed to the reduction of IMR.






